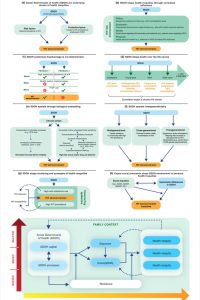
Digital technology can strengthen health systems, improve health financing and public health, and increase reach to underserved populations, according to a new World Bank report launched today. The report also finds that digital technology and data are especially helpful to prevent and manage chronic diseases, care for both young and aging populations, and prepare for future health emergencies and health risks triggered by climate change.
The report, Digital-in-Health: Unlocking the Value for Everyone, was launched today during the G20 Health Ministers Meeting in Gandhinagar, India. It presents a new way of thinking from simple digitization of health data to fully integrating digital technology in health systems: Digital-in-health. This means, for example, infusing digital technologies in health financing, service delivery, diagnostics, medical education, pandemic preparedness, climate and health efforts, nutrition, and aging.
The report also underscores that the successful use of digital technologies must be inclusive of all population groups, and ensure access to digital infrastructure, modern technologies, and skills, especially for vulnerable people.
“Designed with people at the center, digital technology can make health services more personal, prevent healthcare costs from increasing, reduce differences in care, and make the job easier for those who provide health services,” said Mamta Murthi, Vice President for Human Development, World Bank. “We hope that this report will give governments confidence and practical guidance, regardless of the country’s stage of digital maturity or fiscal challenges.”
Improving health is getting harder, not easier. Health systems face serious and growing challenges and policy decisions are too often not based on reliable data. It is estimated that some countries use less than 5% of health data to improve health which means that decisions are not based on data or data is not used effectively to make improvements. Within challenging fiscal environments, people-centered and evidence-based digital investments can help governments save up to 15% of health costs. The report presents pragmatic, low-cost actions to improve digital-in-health, no matter the maturity of a country’s systems or digital infrastructure. For example, better health data governance and standards to ensure systems can readily connect and exchange information are not costly but will be game changing in reducing siloed digital solutions and fragmentation.
“In India, we have shown that digital innovations such as tele-consultations have reached more than 140 million people and provided accessible, affordable and efficient healthcare for everyone,” said Mansukh L Mandaviya, Minister for Health and Family Welfare, India. “We believe a digital-in-health approach can unlock the value of digital technologies and data and has the potential to prevent disease and lower healthcare costs while helping patients monitor and manage chronic conditions.”
To help countries embrace a digital-in-health approach, the report proposes three essential areas to guide investments:
- Prioritizeevidence-based digital investments that tackle the biggest problems and focus on the needs of patients and providers.
- Connect the regulatory, governance, information, and infrastructure dots so that patients know that data is safe and health workers can use digital solutions transparently.
- Scale digital health for the long run based on trust with sustainable financing, and improved capacity and skills for digital solutions.
It will take global, regional, and country leadership to make digital-in-health a reality. The report recommends strong country leadership involving all relevant sectors and stakeholders, including civil society. Digital technology and data improvements will involve investments beyond the health sector and new partnerships with the private sector. A digital-in-health mindset needs to be a routine aspect of annual health system planning, budgeting, and implementation.
The World Bank is committed to helping low-and middle-income countries to make digital-in-health a reality to improve health for everyone. Over the past decade, the World Bank has invested almost $4 billion in digital health including in health information systems, digital governance, identification systems, and infrastructure.
For more information, including a copy of the new report, Digital-in-Health: Unlocking the Value for Everyone, please visit:
Website: www.worldbank.org/en/topic/health
Twitter: http://www.twitter.com/WBG_Health
Facebook: http://www.facebook.com/worldbank
YouTube: http://www.youtube.com/worldbank